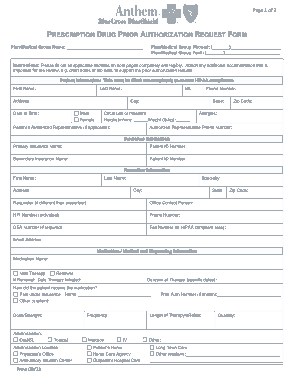
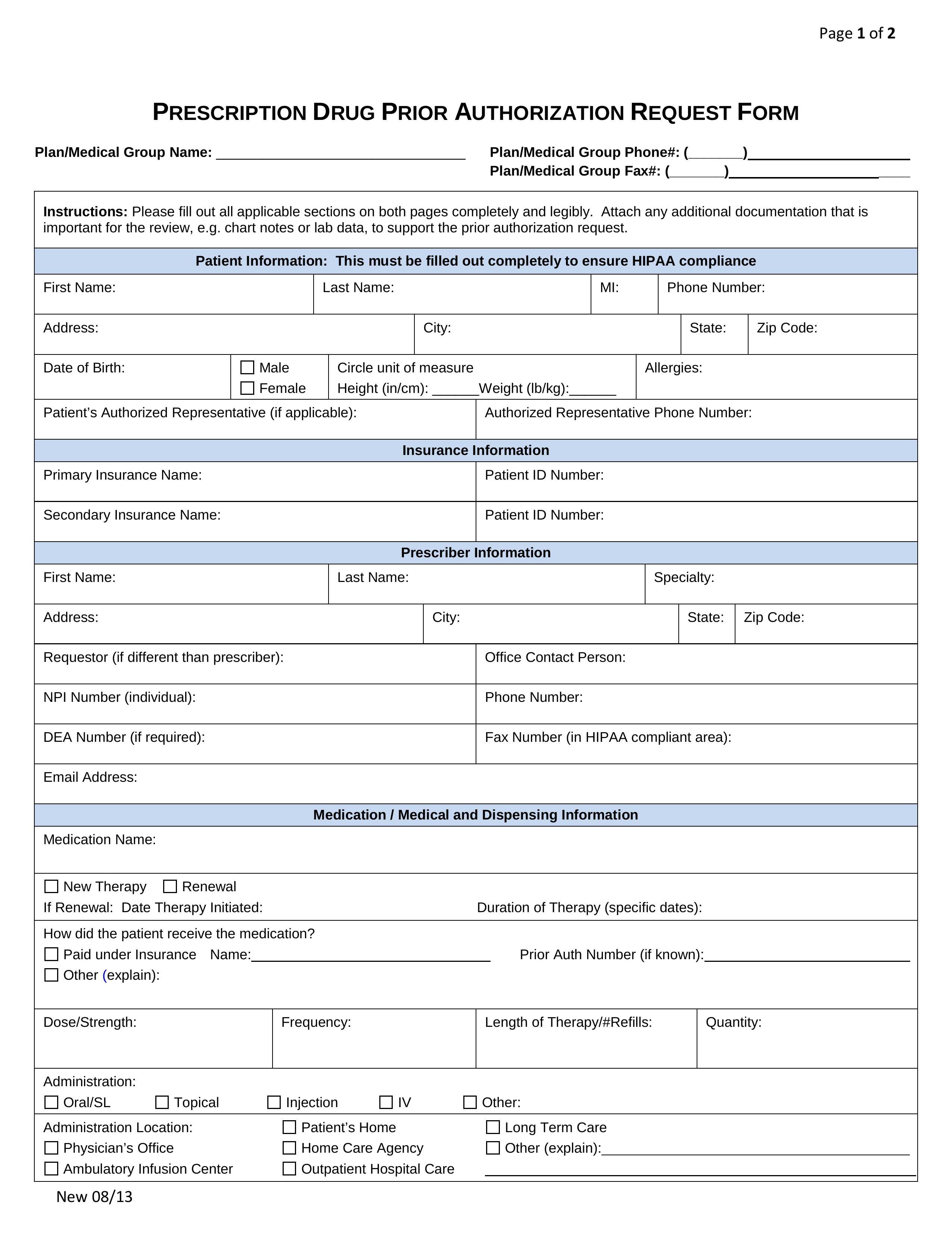
PolicyCriteria Provider must submit documentation such as office chart notes lab results or other clinical information supporting that member has met all approval criteria. The pharmacy can give the member a five day supply.
Http Www Sfhp Org Files Providers Formulary Prior Auth Criteria Pdf
The Participating Group signed below hereby accepts and adopts as its own the criteria for use with Prior Authorization as administered by CVS Caremark.
Vyvanse prior authorization criteria. As part of the PBHMI a prior authorization is required for pediatric members less than 3 years of age who are being prescribed a stimulant medication regardless as to whether or not the stimulant is preferred on the Plans formulary. The Member is at least 18 years of age. It is the policy of health plans affiliated with Centene Corporation that Vyvanse is.
Vyvanse to Treat Binge Eating Disorder Prior Authorization Criteria. Completereview information sign and date. Prior Authorization Criteria Form.
Must not have contraindication listed below Use with monoamine oxidase. 60 Look back timeframe. Prior Authorization Form Amphetamines This fax machine is located in a secure location as required by HIPAA regulations.
PRIOR AUTHORIZATION CRITERIA. Vyvanse Vyvanse is indicated for the treatment of. Request is for a non-formulary agent OR member is currently stable on the requested non-formulary agent see criteria below for non-formulary agents OR B.
Maximum dose is 50 mgday 25 End stage renal disease ESRD. Patient is 13 years of age or older AND Diagnosis of ADHD for Vyvanse only. You may contact Paramount by phone at 1-419-887-2520 with questions regarding the Prior Authorization process.
Maximum dose is 30 mgday 25. Please contact Paramount Advantage at 1-419-887-2520 with questions regarding the Prior Authorization process. Submit charges to Navitus on a Universal Claim Form.
Fax signed forms to Paramount Advantage at 1-844-256-2025. Please contact CVSCaremark at 1-800-294-5979 with questions regarding the prior authorization process. Criteria for prior authorization for stimulant medications prescribed to adults ages 18 or older.
FORMS ARE UPDATED FREQUENTLY AND MAY BE BARCODED. Medication must be prescribed by or in consultation with a psychiatrist or psychiatric nurse practitioner. Inform the member that the medication requires prior authorization by Navitus.
When the following criteria are met. Fax signed forms to CVSCaremark at 1-888-836-0730. Member must meet DSM-V criteria for Binge Eating Disorder BEDincluding ALL of the following.
Texas Prior Authorization Program Clinical Criteria Vyvanse Lisdexamfetamine October 23 2020 Copyright 2013-2020 Health Information Designs LLC 7 Step 5 alternate therapy for BED Required days supply. O Patient must have a documented diagnosis within the previous 365 days of adult ADHD binge eating. Please contact CVSCaremark at 1-800-294-5979 with questions regarding the prior authorization process.
For all requests for Vyvanse all of the following criteria must be met. Criteria for approval bullet points below are all inclusive unless otherwise noted. Diagnosis of ADHD OR adults.
DRUG CLASS AMPHETAMINES. One of the following criteria must be met. During the next business day the prescriber must submit a Prior Authorization Form.
Completereview information sign and date. When conditions are met we will authorize the. Please fax signed forms to Paramount at 1-844-256-2025.
Signature Date Client Name. Member must be 18 years of age or older. Request is for a stimulant with a prescribed quantity that exceeds the.
CNS Stimulants Prior Authorization Request Form Page 1 of 2 DO NOT COPY FOR FUTURE USE. Documented diagnosis of Binge Eating disorder BED AND 2. The member is not responsible for the copay.
When conditions are met we will authorize the coverage of Vyvanse. Vyvanse lisdexamphetamine Vyvanse lisdexamphetamine may be covered for Binge Eating Disorder BED if ALL of the following criteria are met and a PA request to Tufts Health Plan using the Universal Pharmacy Medical Review Request Form is submitted. Attention Deficit Hyperactivity Disorder ADHD Moderate to Severe Binge-Eating Disorder BED in adults COVERAGE CRITERIA The requested drug will be covered with prior authorization when the following criteria are met.
Completereview information sign and date. Vyvanse Authorization guidelines Prior Authorization is required for the following. Patients must meet the following criteria for NON-PREFERRED stimulants.
Prior to treatment assess for presence of cardiac disease 24 Severe renal impairment. Prior Authorization Criteria Form This form applies to Paramount Advantage Members Only Vyvanse Completereview information sign and date. Fax signed forms to CVSCaremark at 1-888-836-0730.
This form applies to Paramount Commercial Select Members Only. 180 days 16353 PROZAC 10MG PULVULE 16354 PROZAC 20MG PULVULE 16355 PROZAC 40MG PULVULE. Patient is 6 years of age or older for Mydayis requests.
You will be reimbursed for the drug cost plus a. Quantity for Approval - Quantity Limit Chart Drug Quantity25 days Quantity75 days Adderall 5 mg 75 mg 10 mg 125 mg 120 tablets 360 tablets. Prior Authorization Form GEHA FEDERAL - STANDARD OPTION Amphetamines This fax machine is located in a secure location as required by HIPAA regulations.
BRAND NAME generic ADDERALL amphetamine mixture ADDERALL XR amphetamine extended -release mixture ADZENYS ER amphetamine extended -release oral suspension ADZENYS XR-ODT amphetamine extended -release orally disintegrating tablets DESOXYN methamphetamine. In addition to the medication-specific criteria below for the non-. Member Information required Provider Information required Member Name.